Respiratory organs
· General body surface: E.g. lower invertebrates like sponges, coelenterates, flatworms etc.
· Skin or moist cuticle (cutaneous respiration):
E.g. earthworms, leech, amphibians etc.
· Tracheal tubes: E.g. insects, centipede, millipede, spider etc.
· Gills (Branchial respiration): E.g. fishes, tadpoles, prawn etc.
· Lungs (Pulmonary respiration): E.g. most vertebrates.
HUMAN RESPIRATORY SYSTEM
It consists of a pair of air passages (air tract) and lungs.
1. Air passages
- Conducting part which transports the atmospheric air into the alveoli, clears it from foreign particles, humidifies and brings the air to body temperature.
External nostrils → nasal passage → nasal chamber (cavity) → nasopharynx (a part of pharynx) → glottis → larynx → trachea → primary bronchi → secondary bronchi → tertiary bronchi → bronchioles → terminal bronchioles → respiratory bronchiole → alveolar duct.
- Each terminal bronchiole gives rise to a number of very thin and vascularised alveoli (in lungs).
- A cartilaginous Larynx (sound box or voice box) helps in sound production.
- During swallowing, epiglottis (a thin elastic cartilaginous flap) closes glottis to prevent entry of food into larynx.
- Trachea, all bronchi and initial bronchioles are supported by incomplete cartilaginous half rings.
2. Lungs
- Situate in thoracic chamber and rest on diaphragm.
- Right lung has 3 lobes whereas left lung has 2 lobes.
- Lungs are covered by double-layered pleura (outer parietal pleura and inner visceral pleura).
- The pleural fluid present in between these 2 layers lubricates the surface of the lungs and prevents friction between the membranes.
- Lungs= Bronchi + bronchioles + alveoli.
- Alveoli and their ducts form the respiratory or exchange part of the respiratory system.
- Alveoli are the structural and functional units of lungs.
Steps of respiration
1. Pulmonary ventilation (breathing).
2. Gas exchange between alveoli & blood.
3. Gas transport (O2 transport & CO2 transport).
4. Gas exchange between blood & tissues.
5. Cellular or tissue respiration.
MECHANISM OF BREATHING
(INSPIRATION & EXPIRATION)
a. Inspiration
- Active intake of air from atmosphere into lungs.
- During this, the diaphragm contracts (flattens) causing an increase in vertical volume (antero-posterior axis).
- Contraction of external inter-costal muscles (muscles found between ribs) lifts up the ribs and sternum causing an increase in thoracic volume in the dorso-ventral axis.
- These changes reduce pressure inside the thorax causing the expansion of lungs. Thus pulmonary volume increases resulting in decrease of intra-pulmonary pressure to less than the atmospheric pressure. So air moves into lungs.
b. Expiration
- Passive expelling of air from the lungs.
- During this, inter-costal muscles & diaphragm relax causing a decrease in thoracic volume and thereby pulmonary volume. So air moves out.
- During forceful expiration, abdominal muscles and internal inter-costal muscles contract.
- Respiratory cycle= an inspiration + an expiration
- Normal respiratory (breathing) rate: 12-16 times/min
- Spirometer (respirometer): To measure respiratory rate.
Respiratory volumes and capacities
- Tidal volume (TV): Volume of air inspired or expired during a normal respiration (volume of air renewed in respiratory system during each breathing). It is about 500 ml.
- Inspiratory reserve volume (IRV) or complemental air: Additional volume of air that can inspire by forceful inspiration. It is about 2500-3000 ml.
- Expiratory reserve volume (ERV) or supplemental air: Additional volume of air that can expire by a forceful expiration. It is about 1000-1100 ml.
- Residual volume (RV): Volume of air remaining in lungs even after a forcible expiration. It is about 1100-1200 ml.
- Inspiratory capacity (IC): Volume of air inspired after a normal expiration (TV + IRV). It is about 3000-3500 ml.
- Expiratory capacity (EC): Volume of air expired after a normal inspiration (TV + ERV). It is about 1500-1600 ml.
- Functional residual capacity (FRC): Volume of air remaining in the lungs after a normal expiration (ERV + RV). It is about 2100-2300 ml.
- Vital capacity (VC): Volume of air that can breathe in after a forced expiration or Volume of air that can breathe out after a forced inspiration (ERV + TV + IRV). It is 3500-4500 ml.
- Total lung capacity (TLC): Total volume of air in the lungs after a maximum inspiration. (RV + ERV + TV + IRV or VC + RV). It is about 5000-6000 ml.
- Part of respiratory tract (from nostrils to terminal bronchi) not involved in gaseous exchange is called dead space. Dead air volume is about 150 ml.
GAS EXCHANGE
Gas exchange occurs between
1. Alveoli and blood 2. Blood and tissues
Alveoli are the primary sites of gas exchange. O2 and CO2 are exchanged in these sites by simple diffusion based on
- Pressure/ concentration gradient
- Solubility of gases
- Thickness of membranes
- Surface area of respiratory membrane (lungs)
The Partial pressures (individual pressure of a gas in a gas mixture) of O2 and CO2 (pO2 and pCO2) are given below.
Respiratory gas
|
pO2 (in mm Hg)
|
pCO2 (in mm Hg)
|
Atmospheric air
|
159
|
0.3
|
Alveoli
|
104
|
40
|
Deoxygenated blood
|
40
|
45
|
Oxygenated blood
|
95
|
40
|
Tissues
|
40
|
45
|
- pO2 in alveoli is more (104 mm Hg) than that in the blood capillaries (40 mm Hg). So O2 diffuses into capillary blood. pCO2 in deoxygenated blood is more (45 mm Hg) than that in the alveolus (40 mm Hg). So CO2 diffuses to alveolus.
- As the solubility of CO2 is 20-25 times higher than that of O2, the amount of CO2 that can diffuse through the diffusion membrane per unit difference in partial pressure is much higher compared to that of O2.
The diffusion membrane is made up of 3 layers:
a) The thin squamous epithelium of alveoli
b) The endothelium of alveolar capillaries and
c) The basement substance between them.
However, its total thickness is much less than a millimetre.
GAS TRANSPORT
(O2 TRANSPORT & CO2 TRANSPORT)
1. Transport of O2: In 2 ways
a. In physical solution (blood plasma): About 3% of O2 is carried in a dissolved state through plasma.
b. As oxyhaemoglobin: About 97% of O2 is transported by RBC. O2 binds with haemoglobin (red coloured iron containing pigment present in the RBCs) to form oxyhaemoglobin. This is called oxygenation. Hb has 4 haem units. So each Hb molecule can carry 4 oxygen molecules. Binding of O2 depends upon pO2, pCO2, H+ ion concentration (pH) and temperature.
- In the alveoli, high pO2, low pCO2, lesser H+ ion concentration and lower temperature exist. These factors are favourable for the formation of oxyhaemoglobin.
- In tissues, low pO2, high pCO2, high H+ ions and high temperature exist. So Hb4O8 dissociates to release O2.
- Every 100 ml of oxygenated blood can deliver around 5 ml of O2 to the tissues under normal physiological conditions.
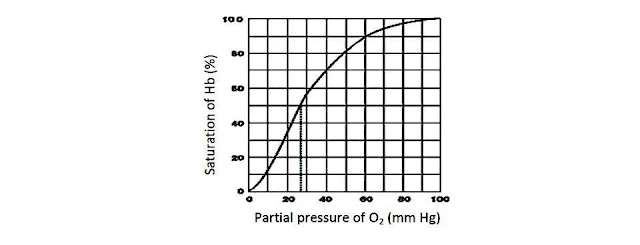
Oxygen-haemoglobin dissociation curve
It is useful to study the effect of factors like pCO2, H+ concentration etc., on binding of O2 with Hb.
2. Transport of CO2: In 3 ways
In tissues, pCO2 is high and pO2 is low. In lungs, pCO2 is low and pO2 is high. This favours CO2 transport from tissues to lungs.
a. As carbonic acid: In tissues, about 7% of CO2 is dissolved in plasma water to form carbonic acid and carried to lungs.
b. As carbamino-haemoglobin: In tissues, 20-25% of CO2 binds to Hb to form carbamino-haemoglobin. In alveoli, CO2 dissociates from carbamino-haemoglobin.
c. As bicarbonates: About 70% of CO2 is transported by this method. RBCs and plasma contain an enzyme, carbonic anhydrase. This enzyme facilitates the following reactions.
In alveoli, the above reaction proceeds in opposite direction leading to the formation of CO2 and H2O.
Every 100 ml of deoxygenated blood delivers about 4 ml of CO2 to the alveoli.
REGULATION OF RESPIRATION
Respiratory centres present in the brain include
· Respiratory rhythm centre (Inspiratory and Expiratory centres): In medulla oblongata.
· Pneumotaxic centre: In Pons. It moderates the functions of the respiratory rhythm centre.
· Chemosensitive area: Seen adjacent to the rhythm centre.
Increase in the concentration of CO2 and H+ activates this centre, which in turn signals rhythm centre. Receptors associated with aortic arch and carotid artery also recognize changes in CO2 and H+ concentration and send necessary signals to the rhythm centre.
DISORDERS OF RESPIRATORY SYSTEM
1. Asthma: Difficulty in breathing causing wheezing due to inflammation of bronchi and bronchioles.
2. Emphysema: Alveolar walls are damaged. It decreases respiratory surface. Major cause is cigarette smoking.
3. Occupational respiratory disorders: Due to exposure of fumes or dust.
a. Silicosis: Due to breathing of silica.

.JPG)

It’s amazing in support of me to truly have a web site that is valuable meant for my knowledge. Health care
ReplyDeletew
ReplyDelete